Gastritis can make every meal feel a bit stressful, wondering what might trigger the burning, bloating, or discomfort next.
The good news is that what you eat (and how you eat) can make a real difference. A gentle, well-planned gastritis diet can help calm irritation in your stomach lining and support healing over time.
We’ll walk through foods that are usually kinder to a sensitive stomach and the ones that tend to make symptoms worse.
Think of it less as a strict “don’t eat this ever again” list and more as a guide to choosing meals that feel soothing instead of painful.
No matter if you’ve just been diagnosed or you’ve been dealing with gastritis for a while, this guide is here to make things simpler.
We’ll talk about everyday food swaps, easy meal ideas, and practical tips you can actually follow in real life, no complicated plans, just realistic steps toward a calmer, more comfortable stomach.
What is Gastritis?
Gastritis is the inflammation or irritation of the stomach lining. It can develop suddenly (acute) or progress slowly over time (chronic).
This condition is often linked to factors such as infection with H. pylori bacteria, frequent use of NSAIDs, alcohol consumption, autoimmune conditions, bile reflux, or severe physical stress such as major illness or injury.
If gastritis isn’t managed correctly, it can lead to complications such as stomach ulcers or anemia.
Common Symptoms of Gastritis
When you’re dealing with gastritis, it helps to know what signs to watch for and how doctors confirm what’s going on. Here’s a simple look at the common symptoms
- Burning or gnawing pain in the upper belly (especially between meals or at night).
- Bloating and fullness after eating even small meals.
- Nausea or vomiting (sometimes with blood or “coffee-ground”–like specks).
- Indigestion or discomfort after eating.
- Loss of appetite or feeling full very quickly.
- Burping or an acid taste in the mouth.
- Black, tarry stools (possible sign of bleeding – needs urgent medical care).
- Fatigue or weakness may indicate anemia developing from long-term irritation or bleeding.
How Gastritis Is Diagnosed?
Before your doctor recommends treatment for gastritis, they first need to confirm what’s actually happening inside your stomach. Here are the main tests and checks they typically use to diagnose gastritis clearly and safely.
- Medical history & symptom review: Your doctor will ask about your pain pattern, triggers, current medications (like ibuprofen or aspirin), alcohol use, and stress levels.
- Physical examination: They gently press on different areas of your stomach to check for tenderness, pain, or swelling.
- Endoscopy (upper GI endoscopy): A thin, flexible tube with a camera is passed through your mouth into your stomach so the doctor can see the stomach lining and, if needed, take small tissue samples (biopsy).
- Tests for H. pylori: A breath or stool test is commonly used to detect Helicobacter pylori infection. In some cases, a biopsy during endoscopy may also be performed.
- Blood tests: These help look for anemia, signs of infection, and other markers of overall health.
- Stool test: This checks for hidden (occult) blood in your stool, which can suggest bleeding in the stomach.
What to Eat With Gastritis
Many experts suggest focusing on gentle carbs, soothing liquids, lean proteins, and well-cooked veggies, along with nutrients that support healing.
1. Easily Digestible Carbohydrates

During a gastritis flare, simple, easy-on-the-stomach carbs are your best friends. Think plain oats, brown or white rice, mashed potatoes, and sweet potatoes.
These give you steady energy without being too heavy. Try to skip greasy, sugary, or highly processed carbs like donuts, fries, and decadent desserts as they can aggravate symptoms and make the burning or bloating worse.
2. Lean Proteins
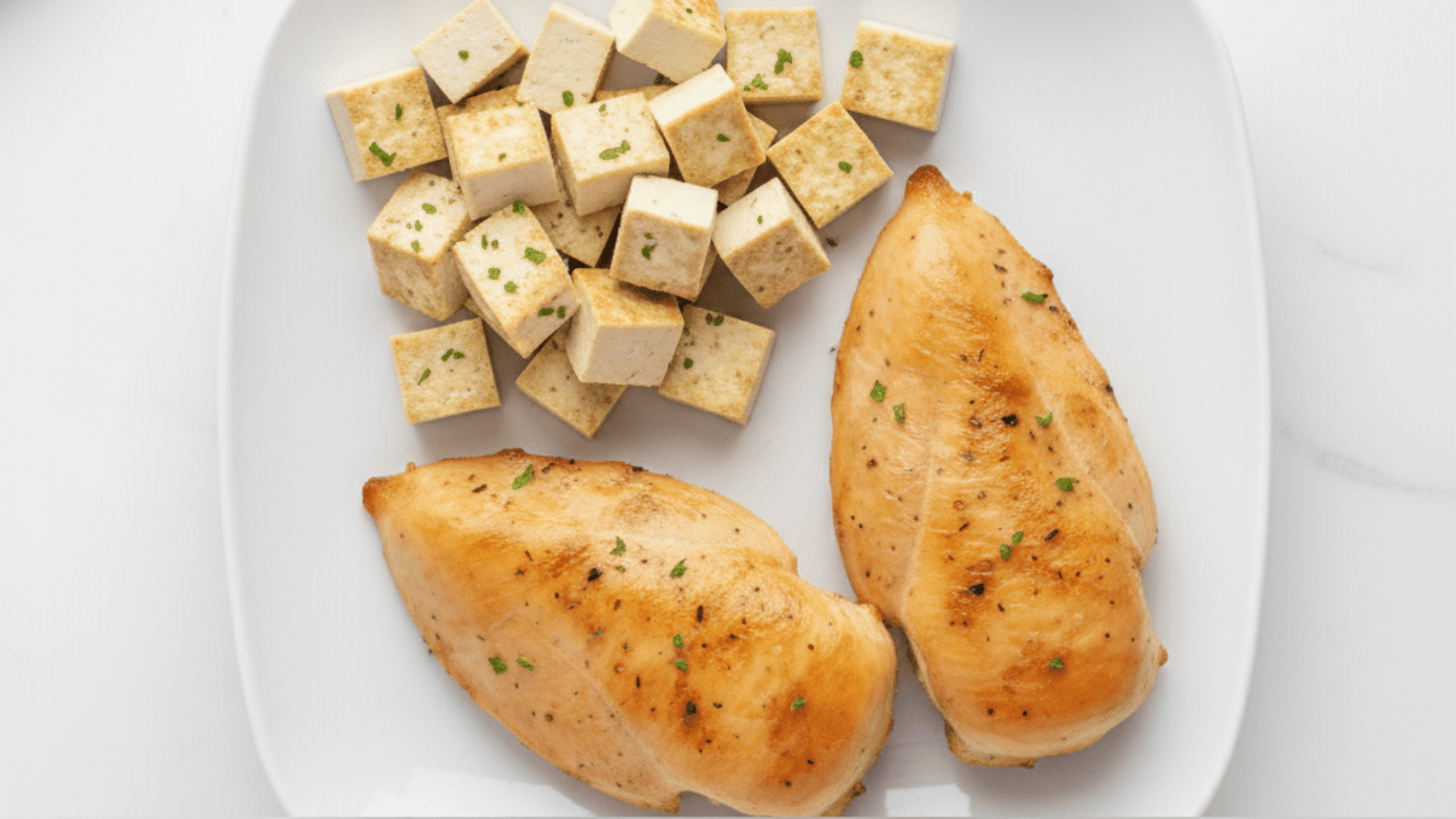
Protein is essential for repair and overall health, but some sources (like fatty or heavily fried meats) can be tough on an inflamed stomach.
Instead, choose gentler options such as baked or steamed fish, skinless chicken, turkey, eggs, or tofu.
These are usually easier to digest and less likely to trigger pain, while still helping your body stay strong and support healing.
3. Cooked Vegetables and Non-acidic Fruits

Veggies are still a must, but how you prepare them matters. Raw salads can feel harsh when your stomach is irritated, so go for steamed, boiled, or lightly sautéed vegetables.
Mild options like carrots, pumpkin, squash, green beans, zucchini, and spinach tend to be kinder on the stomach.
For a bit of natural sweetness, choose non-acidic fruits. Many people tolerate milder fruits like bananas, papaya, pears, and cooked apples better than highly acidic fruits such as oranges or grapefruit.
These are usually better tolerated than citrus fruits or very sour berries, which can worsen irritation.
4. Soothing Beverages and Liquids

Liquids can be a gentle way to get calories and nutrients in. Simple options like warm water, clear soups, and light broths are often well tolerated.
Some people tolerate yogurt or kefir well, especially if they contain probiotics. However, dairy may worsen symptoms for others, so it’s best to monitor your personal tolerance. (as long as dairy doesn’t bother them).
Mild herbal teas like chamomile or ginger (not too strong, and without mint or caffeine) may feel comforting for an irritated stomach.
5. Essential Vitamins and Minerals

In long-term gastritis, especially autoimmune gastritis, or when bleeding occurs, deficiencies in vitamin B12 or iron may develop. Including foods rich in these nutrients can be helpful:
- For Iron: lean meats, eggs, lentils (if tolerated), and iron-fortified cereals.
- For Vitamin B12: eggs, dairy products, fish, and fortified plant milks or cereals.
What to Avoid With Gastritis
When your stomach lining is already inflamed, certain foods and drinks can make the burning, bloating, and nausea much worse.
Avoiding (or at least cutting back on) these triggers can make a big difference in how you feel day to day.
1. Spicy, Acidic, and Heavily Seasoned Foods

Chili powders, hot sauces, green chilies, spicy curries, and heavily seasoned dishes can irritate an already sensitive stomach lining.
Very acidic foods like tomatoes, tomato-based sauces, vinegar-heavy pickles, and citrus fruits or juices may also worsen pain and heartburn for many people with gastritis.
2. High-Fat, Fried, and Greasy Foods

Fried chicken, French fries, burgers, chips, and other greasy fast foods stay in the stomach longer and can increase irritation.
Foods loaded with butter, cream, or cheese can also trigger discomfort, especially during a flare.
Keeping fat intake moderate and choosing baked, grilled, or steamed options is usually easier on your stomach.
3. Caffeine and Alcohol

Coffee (even decaf for some people), strong tea, energy drinks, and cola can stimulate acid production and aggravate symptoms.
Alcohol, whether it’s beer, wine, or spirits, can directly irritate the stomach lining and slow healing, so it’s best avoided or kept to a strict minimum when you’re dealing with gastritis.
4. Carbonated and Sugary Drinks

Fizzy drinks like soda, tonic water, and sparkling soft drinks can cause bloating and discomfort by adding extra gas to your digestive system.
Delightful beverages such as regular soda, energy drinks, and sugary fruit juices can also be harsh on a sensitive stomach and may worsen nausea or cramps.
5. Highly Processed and Irritating Foods

Processed meats (like sausages, hot dogs, and salami), instant noodles, packaged snacks, and foods with lots of additives, artificial flavors, or preservatives can be harder to digest and more irritating for some people with gastritis.
Very rough, hard, or crunchy foods (like overly toasted bread, hard crackers, or nuts) may also feel uncomfortable during a flare, especially if you already have pain or rawness in your stomach.
7-Day Gastritis Diet Plan
This 7-day gastritis diet plan includes simple, gentle meals that may help reduce irritation, ease discomfort, and support a calmer stomach.
| Day | Breakfast | Lunch | Snack | Dinner |
|---|---|---|---|---|
| Day 1 | Oatmeal with sliced banana + chamomile tea | Steamed rice + grilled chicken + boiled carrots | Low-fat yogurt with papaya | Baked fish + mashed potatoes + steamed spinach |
| Day 2 | Scrambled eggs + whole-grain toast + pear slices | Brown rice + steamed zucchini + baked turkey | Banana smoothie with almond milk | Vegetable soup (carrot, pumpkin, spinach) + soft bread |
| Day 3 | Oatmeal with honey + cooked apples | Steamed rice + grilled fish + sautéed green beans | Papaya cubes | Boiled potatoes + baked chicken + steamed carrots |
| Day 4 | Banana, oats, and plant-milk smoothie | Quinoa + grilled chicken + steamed squash | Pear slices with yogurt | Vegetable broth soup + baked fish |
| Day 5 | Scrambled eggs + oatmeal + banana | Rice + turkey breast + steamed spinach | Cooked apple with cinnamon | Sweet potato + grilled fish + boiled green beans |
| Day 6 | Oatmeal with pear slices | Quinoa with cooked vegetables + grilled chicken | Banana | Vegetable soup + baked turkey + mashed potatoes |
| Day 7 | Whole-grain toast + boiled eggs + papaya | Brown rice + baked fish + steamed zucchini | Yogurt smoothie with banana | Steamed chicken + mashed sweet potatoes + spinach |
Use this plan as a starting point, adjust meals to your tolerance, and follow your doctor’s advice for lasting relief.
Simple Tips to Live Better With Gastritis
Small changes in how you eat can be just as important as what you eat. These gentle habits can help your stomach feel calmer and less irritated over time.
- Eat smaller, more frequent meals: Big meals stretch the stomach and can worsen pain. Aim for 4–5 small meals instead.
- Chew slowly and don’t rush: Taking your time helps digestion and reduces the chance of bloating and discomfort.
- Avoid lying down right after eating: Wait at least 2–3 hours before lying flat to reduce acid reflux and burning.
- Limit late-night eating: Heavy dinners close to bedtime can trigger nighttime pain and acid symptoms.
- Track your personal trigger foods: Keep a simple food diary to notice which foods worsen your symptoms, then reduce or avoid those
Wrapping Up
Living with gastritis doesn’t mean you’re stuck with bland food forever; it just means your stomach needs a little extra kindness.
By choosing gentle carbs, lean proteins, cooked veggies, and non-acidic fruits, you can still enjoy satisfying meals without constantly worrying about pain and burning.
Remember, everyone’s triggers are slightly different.
Use this guide as a starting point, then notice how your body responds and adjust from there. And always pair diet changes with your doctor’s advice and prescribed treatment.
Small, consistent choices like eating slowly, avoiding trigger foods, and not skipping meals can make a big difference in how your stomach feels each day.
DisclaimerThis Article is for educational purposes and should not replace professional medical advice. Always consult your doctor for diagnosis and treatment. |
Frequently Asked Questions
Can I Drink Milk If I Have Gastritis?
Some people tolerate low-fat milk; others feel worse. If it triggers bloating or pain, cut back or try lactose-free or plant-based options.
How Long Until I Feel Better with Diet Changes?
Mild gastritis may improve in days to weeks with treatment and a gentle diet, but chronic cases can take longer. Always check with your doctor if symptoms persist.
Is Fasting Good For Gastritis?
Going too long without eating can sometimes make symptoms worse because of increased stomach acid. Instead of long fasts, aim for small, regular meals.













